When to Activate Emergency Response System
If possible, send someone to activate the Emergency Response System, and begin CPR immediately. As soon as it’s available to use an AED. If you’re not with someone (and you do not have a mobile phone), leave the patient to activate the Emergency Response System while also retrieving an AED.
Team Resuscitation: HCP’s can use flexibility when activating the emergency response to fit the provider’s clinical setting, for better management.
Adult and Adolescents CPR
Scene Safety and Recognition of Cardiac Arrest: Check for safety and responsiveness, no breathing, gasping, check pulse for more than 5 seconds but within 10 seconds (breathing and pulse check can occur simultaneously).
Check Pulse: You can test the pulse by placing two fingers on the carotid artery (press your index and 3rd finger on the side of the neck, against the windpipe). You can also check the wrist by placing the same two fingers on the inside of the wrist below the thumb.
C is for Circulation – Adult and Adolescent Compressions
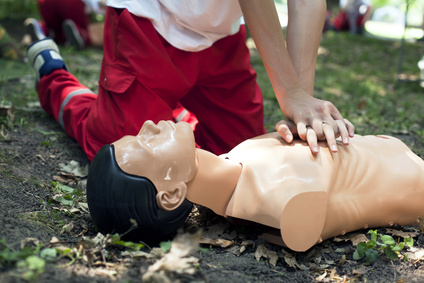
Circulation - chest compressions circulate the blood within the patient. It's important to place your hands correctly upon the patient’s chest. Chest Compression Tempo: perform CPR while matching the tempo of the song, "Staying Alive" while making sure to push hard and fast.
Compression-ventilation ratio without Advanced Airway
Make sure the adult or adolescent is resting upon a firm, solid surface. Perform chest compressions on the lower half of the breastbone (sternum). Once in position, lock your elbows and use your body’s weight to compress at least 2 inches (5 cm) upon the patient’s chest. Do not lean on the patient’s chest in between compressions and make sure the chest ultimately recoils. Limit all interruptions to less than 10 seconds while performing CPR.
It’s important to note: that when performing chest compressions on an adult or adolescent you should compress at least 2 inches (5 cm). The compression rate is 100-120/min. 2 Rescuers: Perform tasks simultaneously. Administer compressions over breathing 30:2.
Chest Compression Fraction: is the total percentage of resuscitation time when performed by the rescuer(s) during cardiac arrest. Whether intended or unintended interruptions (such as real-world delays) occur Chest Compression Fraction aims to minimize pauses in chest compressions. Chest Compression Fraction Goal: target of at least 60%.
Compression-ventilation ratio with Advanced Airway
- Continuous compressions at a rate of 100-120/min
- One breath every 6 seconds (10 breaths/min)
A is for Airway - Clear the Airway
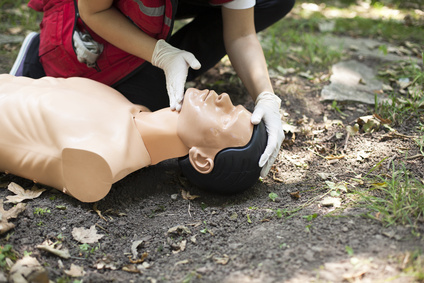
Airway - Make sure the patient is on a solid surface (on the backside). Next, kneel next to the patient’s neck and shoulders. Open the patient’s airway by tilting the head back with the palm of one hand while gently lifting the chin with your other hand. For no more than 10 seconds, check for life: listen for any sounds, put your cheek next to the patient’s mouth to feel any breaths while also looking for any motion. Rescuers can check steps simultaneously. If the patient is assumed lifeless begin Mouth-to-Mouth procedure.
Jaw-Thrust Maneuver: 1. Kneel above the patient’s head. 2. Rest your elbows on the surface. 3. Place one hand on both sides of the patient’s jaw. 4. Stabilize the patient’s head with your forearms. 5. Use your index finger to lower the patient’s jaw as you use your thumb to retract the patient’s lower lip. If the patient is assumed lifeless, perform mouth-to-mouth.
B is for Breathing - Mouth-to-Mouth
Rescue Breathing is widely known to be performed mouth-to-mouth—it can also be performed mouth-to-nose but in rare cases. While still performing the Airway technique pinch the patient’s nose shut. With a complete seal over the patient’s mouth, with your mouth, breathe until you see the chest inflate. If the chest does not rise, repeat the Airway technique. Once the chest swells, breathe into the patient a second time (30:2).
Once the breathing technique is applied, continue Circulation, Airway, Breathing (C-A-B’s).
CPR on obese patients
Yes, perform Chest Compressions
CPR on pregnant patients
Yes, perform Chest Compressions and a modification if the pregnant woman’s fundus height (baby-bump) is at or above the level of the umbilicus. If the woman’s fundus height is at or above the umbilicus, then High-quality CPR with manual left uterine displacement will be beneficial for relieving aortocaval compression during, the chest compression task. To perform manual left uterine displacement: push the uterus to the patient’s left side with 1 hand while still providing CPR.
Oxygenation and airway management should be prioritized during resuscitation from cardiac arrest in pregnancy because pregnant patients are more prone to hypoxia.
Fetal monitoring should not be undertaken during cardiac arrest in pregnancy because of potential interference with maternal resuscitation.
Opioid poisoning CPR for healthcare providers
1. Suspected opioid poisoning
- Check for responsiveness
- Shout for nearby help
- Activate the emergency response system
- Get naloxone and an AED if available
If yes, prevent deterioration:
- Tap and shout
- Open the airway and reposition
- Consider naloxone
- Transport to the hospital
If no, does the patient have a pulse? Assess for 10 seconds.
If yes, support ventilation:
- Open the airway and reposition
- Provide rescue breathing or bad-mask device
- Give naxolone
If no, start CPR:
- Use an AED
- Consider naloxone
- Use high-quality CPR
Rescuers Should Never
- Compress slower than 100/min or faster than 120/min
- Compress in-depth less than 2 inches (5 cm) or more than 2.4 (6 cm)
- Lean on victim’s chest during compressions
- Allow interruption during compressions more than 10 seconds
- Provide excessive ventilation during breathing task, ie., excessive breathing with force or too many breaths
- Check the environment – making sure it’s safe for rescuers and victims
- Check responsiveness
- No breathing or only gasping – ie., no normal breathing
- Within 10 seconds – no positive pulse
- (You can check for a pulse and breathing simultaneously in less than 10 seconds)
- If you do not have a mobile phone – leave the victim and activate the emergency response system while retrieving an AED before performing CPR.
- Have someone activate the emergency response system. Perform CPR immediately and use the AED as it becomes available.
- 1 or 2 rescuers – 30:2
- Chest compressions – 100-120/min
- Give 1 breath every 6 seconds (10 breaths/min)
- 100-120/min
- At least 2 inches (5 cm)
- 2 hands on the breastbone (sternum) on the lower half
- Make sure not to lean on the chest of the victim – Allow a full recoil after each chest compression
- Compression interruptions – limit to less than 10 seconds
- Compress slower than 100/min or faster than 120/min
- Compress in-depth less than 2 inches (5 cm) or more than 2.4 (6 cm)
- Lean on victim’s chest during compressions
- Allow interruption during compressions more than 10 seconds
- Provide excessive ventilation during breathing task, ie., excessive breathing with force or too many breaths